A car accident, the loss of a loved one and financial trouble are just a few of the myriad stressors we may encounter in our lifetimes. Some of us take it in stride, while others go on to develop anxiety or depression. How well will we deal with the inevitable lows of life?
A clue to this answer, according to a new Duke University study, is found in an almond-shaped structure deep within our brains: the amygdala. By measuring activity of this area, which is crucial for detecting and responding to danger, researchers say they can tell who will become depressed or anxious in response to stressful life events, as far as four years down the road.
Published Feb. 4, 2015, in Neuron, the results may eventually lead to new strategies to treat depression and anxiety and prevent them from occurring in the first place.
“Often, individuals only access treatment when depression and anxiety has become so chronic and difficult to live with that it forces them to go to a clinic,” said the study’s first author Johnna Swartz, a Duke postdoctoral researcher in the lab of senior author Ahmad Hariri. “With a brain marker, we could potentially guide people to seek treatment earlier on, before the disorders become so life altering and disruptive that the person can’t go on.”
Small studies of people at risk for post-traumatic stress disorder (PTSD), such as soldiers deployed to combat zones, have hinted at the link between individual differences in brain activity and the ability to handle stressors.
Those studies also focused on the amygdala -- for its established link to psychiatric disorders including PTSD, anxiety and depression -- but included participants who had endured highly traumatic events such as active combat. In contrast, most people in the general population experience less severe forms of stress, such as unemployment, divorce, or a death in the family.
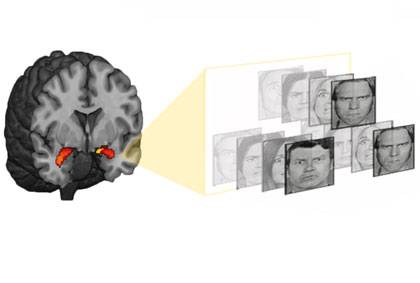
In the new study, Hariri’s team scanned the brains of healthy college students as they looked at angry or fearful faces, which signal danger in our environment. These threatening pictures normally trigger the amygdala, and the scientists measured the intensity of this activation using functional magnetic resonance imaging, a noninvasive, indirect measure of brain activity.
Every three months after the scan, participants completed an online survey documenting stressful life events and their impact, as well as a questionnaire that assessed symptoms of depression and anxiety.
From the initial 753 participants who were scanned, nearly 200 completed the online surveys an average of two years, and as long as four years, after the scan. In these individuals, the more reactive the amygdala was at the study’s start, the more severe their symptoms of anxiety or depression in response to stressful events they encountered after scanning.
Importantly, the participants who had an overzealous amygdala but who had not experienced recent stress did not show these elevations in symptoms.
“To find that a single measure of the brain can tell us something important about a person’s psychological vulnerability to stress up to four years later is really remarkable and novel,” said Hariri, a professor of psychology and neuroscience and a member of the Duke Institute for Brain Sciences.
The ability for the brain marker to predict symptoms was surprising, Hariri said, given that the population was healthy and, for the most part, dealing with normal and relatively mild stressors for young adults, like an argument with a parent, or problems at work or school.
The new research is part of the Duke Neurogenetics Study, a long-term collection of data on genes, brain activity, environmental factors and symptoms related to psychiatric disorders. The ultimate goal is to understand why some people are more vulnerable to developing depression, anxiety and other mental health problems.
Hariri and his team are continuing to follow their study participants. “We want to know just how far in the future knowing something about an individual’s brain helps us understand their risk,” he said.
The group is also exploring other measures, such as a person’s genes, to predict the differences in amygdala activity, and in turn, the relative risk for anxiety and depression.
Isolating a person’s DNA from a saliva sample and looking for specific differences in its letter code is easier and less expensive than having them undergo a brain scan. Thus, a genetic screen that tells us about a person’s amygdala reactivity is more likely to be available and useful for doctors working to prevent mental illness in their patients, Hariri said.
This research was supported by Duke University, the National Institutes of Health (DA033369, DA031579, P30DA023026), and the National Institute of Child Health and Human Development (T32-HD07376). The text of the journal article is available here in DukeSpace, the university's online repository of open-access research.