Improving Community Health by Addressing Social Stressors
Duke-Margolis study finds pilot projects across NC appear to improve health outcomes and lower costs
“It’s offering a larger array of health-related social needs services than other programs – 29 to be exact – and it’s offering them to a larger population of Medicaid members than other programs,” Bleser added. “It is paying local community-based organizations – not clinicians – to provide the services. And there’s a separate pot of federal dollars to pay for it, with the goal of testing what works at scale to improve health and reduce health care costs. Other states and commercial insurers are eagerly watching to learn what’s working or not in program design and implementation – some are even proposing to do what NC Medicaid is doing – and that’s where our research comes in.”
Researchers from the Duke-Margolis Center for Health Policy analyzed the Pilots program, which endeavors to connect health care and community-based social service providers who work together to assist Medicaid enrollees.
In 2018, the Centers for Medicare & Medicaid Services (CMS) authorized up to $650 million to fund the Pilots, with up to $100 million earmarked to build the capacity of about 150 local community-based social service providers and the three regional community care hub organizations coordinating them.
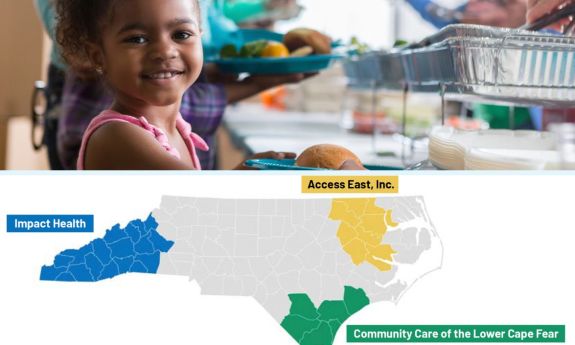
The Pilots were set up in three regions, each overseen by a community care hub: Access East, Inc., in Greenville; Impact Health in western North Carolina; and Community Care of the Lower Cape Fear in Wilmington. They supply 29 evidence-based services in these projects through local community health providers that address health-related social needs.
“The program wasn't planned to have a rural focus, but by chance, the three organizations they competitively selected to run the program – from nine applicants –- happened to comprise mostly rural areas,” said Bleser, one of eight co-authors of the report, six of whom are Duke-Margolis researchers.
Last year, the Duke-Margolis researchers gathered feedback from North Carolina Medicaid members who received Pilots services. The participants “expressed high satisfaction and gratitude for the food services they had received,” and received “clearer communication about service options and more food choices,” according to the report.
On housing, participants were interested in supportive services for homeowners and renters, such as help with air conditioning and heating repairs.
Predictably, the residents who live in the more rural areas of the state pointed to “large gaps in the availability of public transportation,” and inquired about personal vehicle repairs. Their concerns underscored how the lack of a functioning vehicle and public transportation limits their access to the services.
The Pilots funding arrived at a fortuitous time. North Carolina in March became the 40th state to expand Medicaid under the Affordable Care Act. The expansion was stalled for more than a decade, and as a consequence left hundreds of thousands of low-income North Carolinians without access to health care.
Bleser says the implementation of Medicaid expansion does not mean the Pilots are no longer warranted.
“I see Medicaid expansion as complementary to the goals and impacts of the [Healthy Opportunities] Pilots,” he said. “Medicaid expansion means more North Carolinians will be eligible for health-related [support] through the Pilots.”
The Pilots program is set to expire in October 2024. Bleser said state officials applied to renew the program for another five years and expand the program statewide, as well as request new services such as childcare support, firearm safety and mortgage assistance.
Support for the Duke study began with a grant from the Robert Wood Johnson Foundation and a grant last year from the Kate B. Reynolds Charitable Trust to continue and expand the Duke-Margolis researchers’ work.