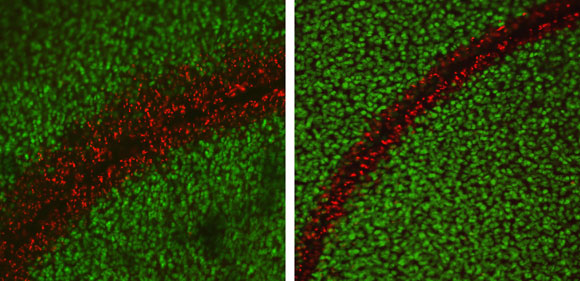
A molecule found in tarantula venom, the peptide GsMTx4, protects against cell death (in red) in a tissue model of cartilage injury.
We live with the same cartilage -- the tissue that connects our joints -- for a lifetime. And since we can’t readily make new cartilage cells, we had better figure out how to keep what we have healthy. Duke scientists and their collaborators have come a step closer to understanding how cartilage senses injury-causing mechanical strain at the cellular level: a pair of channels that work together to cause cartilage cells to die off in droves. Using a substance found in tarantula venom to block these channels, the researchers have prevented cell death caused when cartilage experiences mechanical strain. Published Nov. 10 in the Proceedings of the National Academy of Sciences, the new findings could lead to potential drug targets for protecting joints and preventing the pain associated with cartilage injuries.“The most exciting thing about this study was that it shows that cells in your cartilage, which people don’t think of as a typical sensory cell, have multiple sensory systems,” said Farshid Guilak, the Laszlo Ormandy Professor of Orthopaedic Surgery at Duke and one of the study’s senior authors.“These cells are very complex in their ability to sense their mechanical environment,” said Guilak, who performed this research with Wolfgang Liedtke, M.D. Ph.D., an associate professor of neurology, anesthesiology and neurobiology at Duke University School of Medicine. Joint injury affects millions of people and is caused by traumatic events such as falls, sports injuries, and infections, and the more insidious everyday wear and tear on our cartilage. Compared with other tissues, however, cartilage is slower to heal, because it doesn’t have its own blood supply. And its cells, called chondrocytes, can no longer divide once they become mature.Physical activity is good for cartilage. Earlier this year, Guilak, Liedtke and their collaborators discovered that gentle mechanical stimulation of cartilage cells (similar to that experienced during mild exercise) promotes their health by activating the ion channel TRPV4. A parallel line of evidence showed that mice lacking TRPV4 channels are more likely to develop osteoarthritis.In the new study, Liedtke’s and Guilak’s labs joined again, this time to investigate the response of chondrocytes to more strenuous mechanical stress. They discovered the presence and role of two more mechanically-sensing ion channels, Piezo1 and Piezo2, on cartilage cells.The Piezo channels have gained visibility for their ability to directly transduce mechanical force. For example, Piezo1 is critical for sensing a full urinary bladder. Piezo2 helps us sense gentle touch. Although both Piezo channels are important in a variety of organisms -- including single-cell protozoa and plants -- no one had looked for them in joints, said Liedtke, who is also an attending physician in the Duke Pain Clinics and a member of the Duke Institute for Brain Sciences.Indeed, both channels were present, and they were active in chondrocytes when postdoctoral researcher Whasil Lee compressed the cells using a customized atomic force microscope. Unlike in other tissues however, the channels responded together. They responded not to gentle pressure but to the kinds of compressions that would cause cartilage injury. The researchers wanted to see if inhibiting the Piezo channels would prevent cell death. Luckily, three years earlier, co-author Frederick Sachs and his colleagues from State University of New York, Buffalo, had discovered that a small peptide found in tarantula venom, called GsMTx4, blocks Piezo1 channels. In the new study, synthetic GsMTx4 from Sachs’ lab blocked both channels and protected joint tissue living in a petri dish from cell death following compressive injury. In addition, knocking out each Piezo channel using gene expression interference made individual chondrocytes more resilient to forceful compression.The group was also able to boost potency of GsMTx4 in protecting chondrocytes by adding a chemical that caused Piezo channels to stay on the cell surface for longer time periods, effectively desensitizing them, Liedtke said.The scientists plan to do more basic and translational studies to reveal how exactly Piezo1 and Piezo2 work together, the role of these channels (and GsMTx4) in a living animal, and whether their finding can be used for treatment of post-traumatic joint injury and joint pain.The work was supported by the National Institutes of Health (AR048182, DE018549, DE018549S2 (Administrative Supplement sustained by the American Recovery and Reinvestment Act), R01HL054887, AG15768, AR50245, AR48852, AG46927, and EB002025).Other authors on the study include Duke’s Holly Leddy, Yong Chen, Suk Hee Lee, Nicole Zelenski, Amy McNulty, Jason Wu, Jeffrey Coles, Stefan Zauscher and Jörg Grandl, and Kellie Beicker of the University of North Carolina at Chapel Hill.